Crouched over the kitchen sink, I surged with a repressed groan, stifling the convulsive impulse as tears broke free; I cried, uncontained, momentarily unaware why. I was so used to keeping it in, I had become disconnected from what I was actually feeling — ironic, because what I was feeling right then was disconnected.
I did not recognize my body. This vessel in which I was contained made no sense to me at all. It responded to my thoughts and commands, but it felt completely foreign. Looking down at my arms, my hands, my fingers, I recognized nothing. They could hold the dishes I was washing, turn the knob on the faucet, even scrub with the brush. But there was a clumsiness about them, an awkwardness that was hard to explain or rationalize, except to know immediately that none of that was part of my body. None of it was Me.
Such is the effect of bodily changes that occur under cancer treatment. I was experiencing a slight case of dysmorphia, that feeling of certainty that you are not in the right body. It passed, but the emotional impact lingered.
Let It Bleed — My Skin Has Never Been Thinner
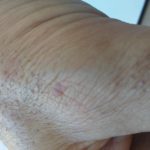
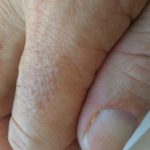
My t-shirts are all dotted with spots of dry blood. My fingertips are split and refuse to heal quickly. When I wash my face, it looks like I scrubbed with barbed wire. Three-plus years of cancer treatment has left me a bit raw.
I wrote those words several months ago, in what seems like another life. The drug I had been taking affected epidural cells and caused a rash that covered my body in acne. It was my first “targeted” therapy and the first treatment to follow my chemotherapy. At the time, I did not realize that treatment was not working — nor did I anticipate that the rash I was describing would be so totally eclipsed by the one I have now. The flip side now is that, while the rash I just endured for eight weeks has been far more viscerally gruesome and painful, the treatment has also offered clear benefits far exceeding any of the protocols used to this point.
Hindsight is always interesting. I recall thinking how horrible my afatinib rash was back in the waning months of last year. Now it seems quaint, the way it came in spots, slowly spreading, and offered its meager challenges in management and mitigation. My dermatologist did her best, offering a range of medicated salves, antibiotic ointments, and even an anti-fungal shampoo, all in an attempt at navigating uncharted territory. Some of it paid off, too; my afatinib-induced rash faded, became more manageable, and quickly vanished once we realized that treatment had failed and the pills were stopped.
By the time I had gone through a second failed targeted therapy and jumped through the hoops for my current clinical trial, my cancer had grown considerably. Not only had the primary tumor increased dramatically in size, but there had been substantial spread in my left lung (and presumably throughout the body). I was ready, determined even, to hit the cancer hard with my treatment. Agreeing to the maximum available dose appeared like the logical choice. After all, I was still relatively healthy and in good shape, in spite of my recent weight loss brought on by radiation and the stomach flu. I was ready and determined to take whatever they were able to give me. But I wasn’t really prepared for that rash.
What If?
I have already described how painful and hideous the first month was on my treatment of poziotinib. But this was balanced by the drug’s efficacy, offering me the first, unwelcome taste of that demon, Hope.
I began to think, what if I could stay on this drug? What if it can kill the cancer entirely, keep it away, maybe even… cure me? What if?
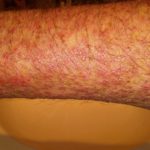
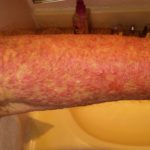
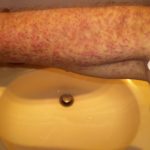
Then, of course, the second month of treatment was every bit as difficult as the first. In different ways, it took its toll. The rash slowly stabilized, at least insofar as it was less painful and more predictable, but it continued to spread. The itching was still crazy — I was going through a pound of skin cream every week in addition to various lotions, oils, and a steroid gel. It seemed borderline insane to spend an hour of my day moisturizing my body, but that was what I was doing.
My body was also fighting the rash consistently, burning all my excess calories, and I continued to lose weight. Touching my skin, it felt hot, but giving off all that heat made me chilly even on a hot, summer day. Every day, I would try to eat extra, but it seemed like I was dieting. Later, there would be nausea, too; vomiting from the combination of drugs I was taking, and adjustments to make everything work. But at first, the loss was strictly tied to the fact that the skin, being the body’s biggest organ, was just using up the most energy.
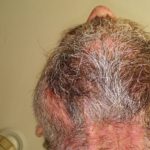
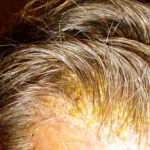
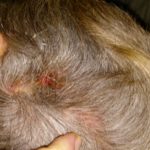
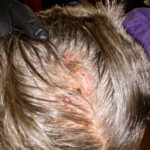
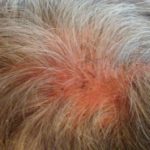
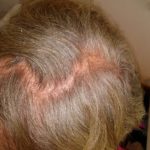
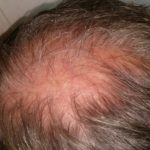
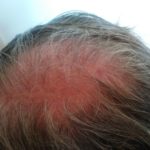
My hair and scalp no longer hurt so much, but the scabbing and itching was giving way to a heavy amount of fall-out. Even my beard was beginning to thin as the hairs would scrape away with the crystalized gunk accumulating around the follicles. And those “what-ifs” spurned by Hope were giving way to the “what-ifs” of failure to maintain the treatment. What if I could not continue doing this? What if I stop and the cancer grows back more quickly than ever? What if there is nothing that will ever be this effective again? These are nasty thoughts, but they haunt me when I look in the mirror. Even now, after two weeks of rest to reduce the rash.
Reassessed
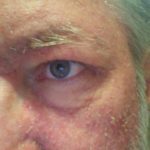
When I went in for my eight-week checkup, it was clear that I was suffering too much from the rash. Even with the antibiotic, I was taking to mitigate its effects, it was covering me from head to toe, and I was in constant discomfort. My oncologist took one look at the extent of the spread and said I had suffered too much and needed a break.
I also had this unexpected development of frequent night cramping in my legs. I have had this on occasion as long as I can remember, waking in the night every so often with a cramp in my arch or my calf, massaging it out and going back to sleep. And I have had restless legs for years, too. But suddenly, I was waking in excruciating pain, one or both legs cramping up at the same time, both the calf and shin, the ankle, the arch of my foot, even my toes.
The joints would twist, the muscles would seize, and I would hold back tears or a scream and try to wait it out. Five minutes. Ten minutes. Two or three times a night. Four, five, even six nights a week. I was put on ropinirole, a drug for Parkinson’s disease and restless leg syndrome; it took a couple of nights to kick in, but it made it possible to sleep again. It also made me nauseous, even more so when combined with the antibiotic I took to fend off the acne. But most of that would be dealt with over the course of my break. Two weeks.
During that time, the rash did begin to clear up. It went from a “stage 3” (really, really bad) to a “stage 1” (not so bad). But I also developed a persistent and increasing cough that was leaving me short of breath and even more tired than before. It has been determined, at least for now, that it is caused by sinusitis — my consistently dripping nose — and is being treated accordingly, with new antibiotics. And while I do that, back into the breach I go.
At least we are doing it with a dose reduction. The dosing in this trial is being done in increments, and I’m knocking down from the maximum of 16mg to the next tier of 14mg, hoping that the small difference in dose translates to a large difference in the persistence of the rash. And then we are back into a monthly routine, taking my daily pills and getting reassessed as we go.
And the lesson of this tale is…
But I skipped the best part of the story, the reason that I am continuing after my two-week break. After the first four weeks, there had been a marked reduction in tumor size, easily on par with or exceeding the initial three-month blast of chemotherapy I completed back in 2015 before going into my long maintenance run on Alimta.
The second four weeks of poziotinib, enduring the rash and all, resulted in an even more amazing continuation of that reduction. While I don’t have a picture of it this time, the tumor was dramatically smaller and had begun to peel away from the chest wall where it had been previously attached. Now, it is a fraction of the size from the last scan — still present, but greatly diminished. And the rest of the lungs look more clear than I have seen them in years.
It’s ironic, I suppose, that the majority of my hair-loss has occurred during the two-week hiatus I took from treatment to clear out the rash. I expect that I’ll continue losing more now that I am re-starting the program, even at the reduced dose. But it feels strangely right, maybe because of the summer heat, maybe because I’ve just been getting used to the feel of my scalp, and it certainly is a small concession to make for such promise.
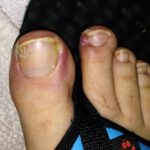
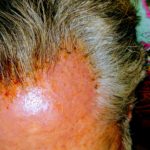
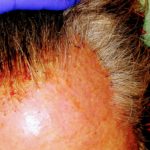
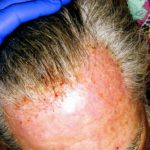
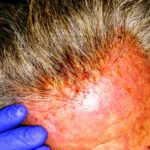
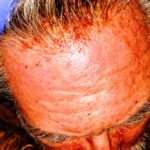
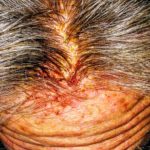
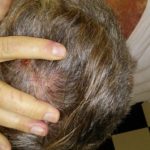
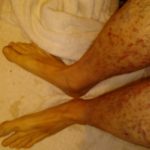
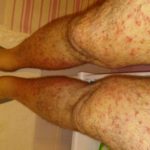
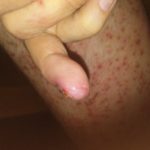
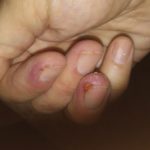
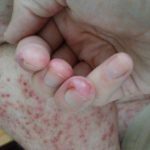
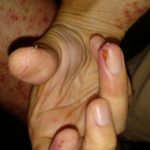
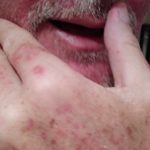
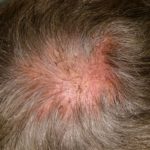
Enjoy the gallery of images from my second month of treatment!
If this post resonates with you, please consider supporting my work through a monthly subscription to my feed on Patreon, or a one-time donation through PayPal. Follow me on Twitter, Facebook, Tumbler and many other fancy social sites or apps. Please share my posts to groups you are involved with on Reddit or Google+ or anywhere else that you feel it will help or enlighten or inspire another reader. (Sharing buttons are below the post!)
Thank you!



























1 thought on “This Is Not My Body”